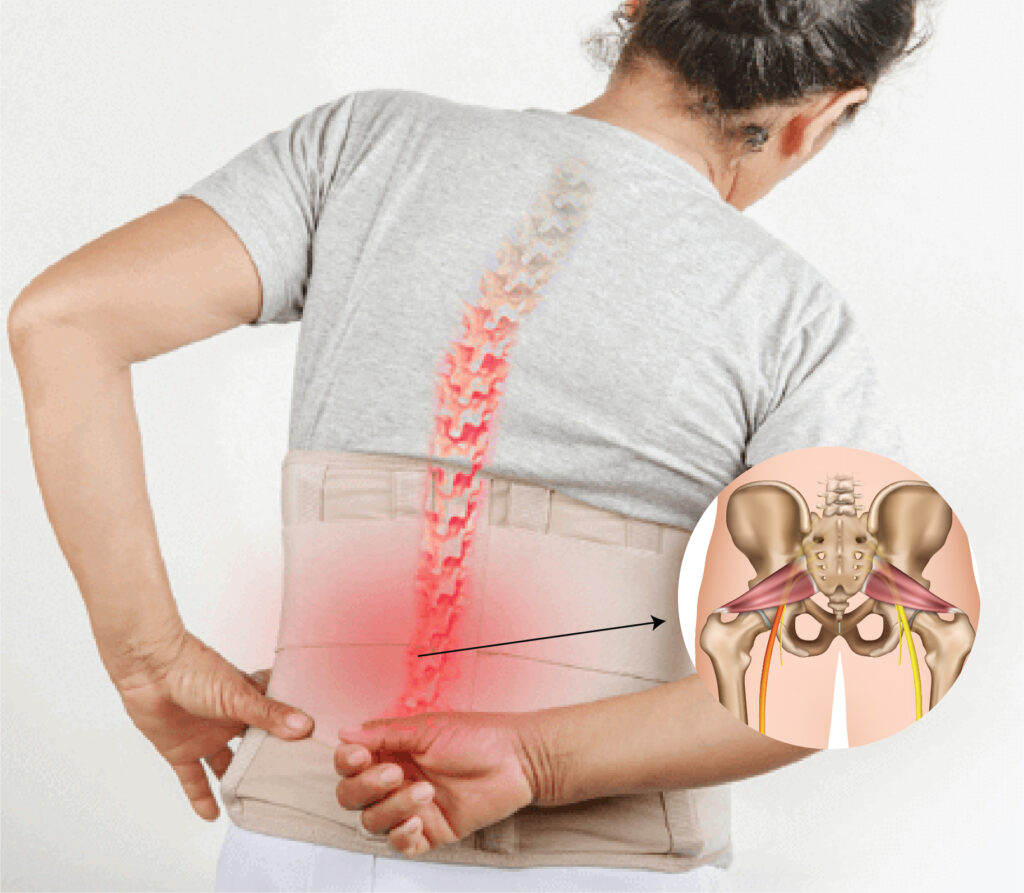
Lumbarisation and sacralisation are anatomical variations in the human spine. Lumbarisation occurs when the last lumbar vertebra resembles a transitional vertebra, resembling the first sacral vertebra. This condition results in an extra lumbar-like segment in the spine. On the other hand, sacralisation involves the fusion of the last lumbar vertebra with the first sacral vertebra, leading to a reduced number of lumbar vertebrae. These variations can manifest as lower back pain or altered biomechanics, impacting an individual’s spinal structure and potentially influencing associated physiological functions. Understanding lumbarisation and sacralisation is crucial for healthcare professionals in diagnosing and addressing related spinal issues.
Symptoms
Symptoms of lumbarisation and sacralisation may include lower back pain, stiffness, and discomfort. Individuals with these anatomical variations may experience altered biomechanics, leading to potential issues such as sciatica, muscle imbalances, and reduced flexibility. Management typically involves targeted exercises, physical therapy, and, in severe cases, surgical intervention.
Causes
Lumbarisation and sacralisation are primarily caused by congenital anomalies during fetal development. Genetic factors and environmental influences can contribute to these variations in the formation of the spine. The abnormal fusion or separation of vertebrae during embryonic stages leads to lumbarisation or sacralisation, influencing the structure of the lower spine.
Rehabilitation
Rehabilitation for lumbarisation and sacralisation focuses on relieving pain, improving flexibility, and strengthening the affected area. Physical therapy exercises, such as core strengthening and targeted stretches, can help address muscle imbalances. Additionally, lifestyle modifications, ergonomic adjustments, and, in some cases, pain management techniques may be incorporated to enhance overall spinal health.
Lumbarisation and Sacralisation F&Q
Lumbarisation and sacralisation are anatomical variations in the spine where certain vertebrae exhibit abnormal characteristics, affecting the structure of the lower back.
Symptoms may include lower back pain, stiffness, sciatica, muscle imbalances, and reduced flexibility due to altered spinal biomechanics.
These variations result from congenital anomalies during fetal development, influenced by genetic factors and environmental conditions that affect the formation of vertebrae.
Rehabilitation typically involves physical therapy exercises, core strengthening, targeted stretches, and lifestyle modifications to alleviate pain, improve flexibility, and address muscle imbalances.
Yes, in many cases, non-surgical interventions such as physical therapy, exercise, ergonomic adjustments, and pain management techniques can effectively manage symptoms and improve spinal health.
Healthcare professionals need to comprehend these variations to diagnose and address associated spinal issues, tailoring interventions to alleviate symptoms and enhance the overall well-being of affected individuals.